MIT Scientists Discover Gut Protein That Traps Bacteria and Strengthens the Intestinal Barrier — Potential Therapy for IBD
Intelectin-2, a lectin found throughout the gastrointestinal tract, was shown in Nature Communications to bind to bacteria's sugar coat and also crosslink mucin proteins to reinforce the mucus barrier, acting as a dual-purpose defender that could inspire new treatments for inflammatory bowel disease.
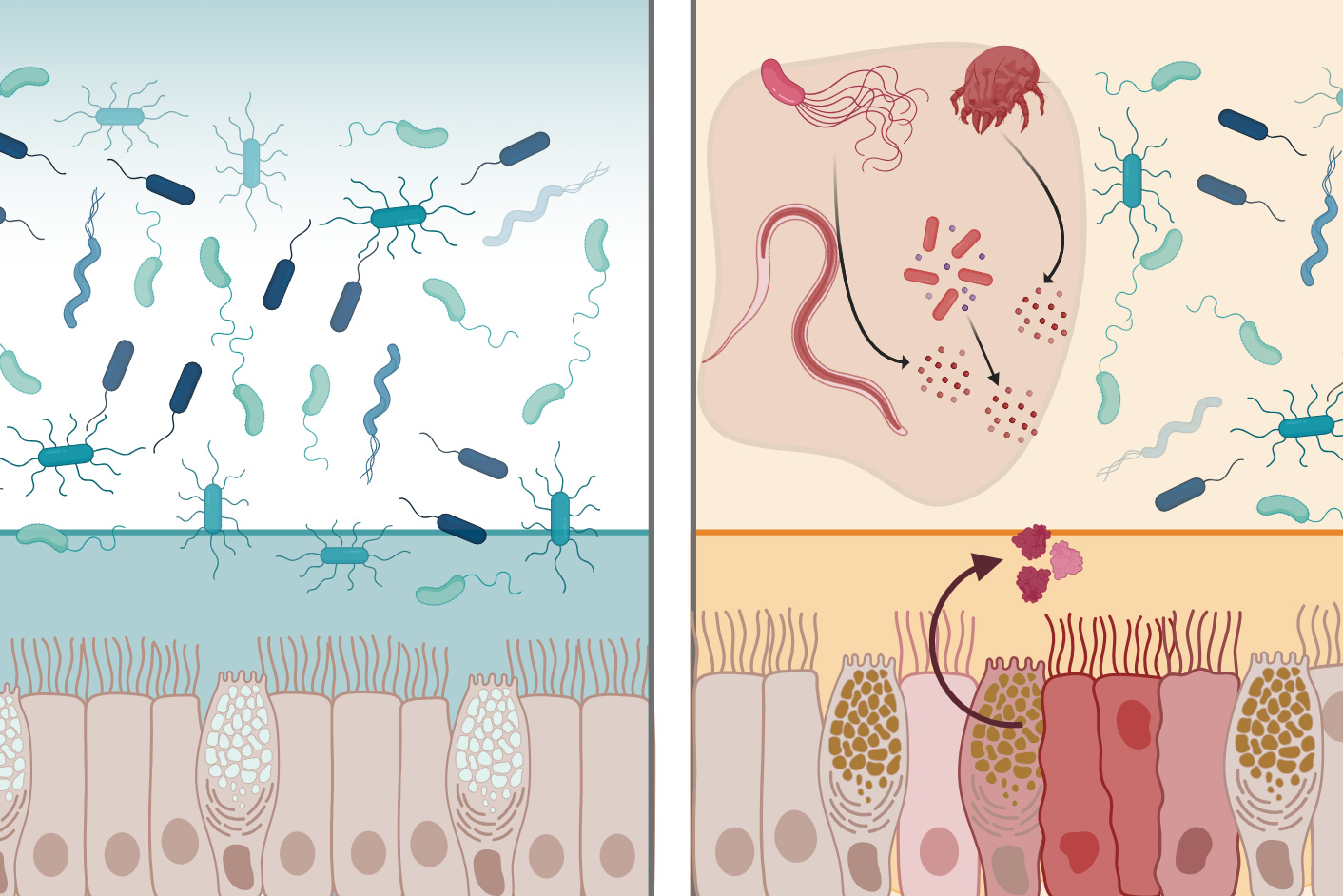
MIT chemists have identified a previously overlooked protein in the gastrointestinal tract with remarkable antimicrobial properties, revealing that a molecule called intelectin-2 performs two distinct defensive functions simultaneously: it binds to sugar molecules on the surface of harmful bacteria, trapping and disabling them, while also crosslinking the mucin proteins that make up the intestinal mucus layer, reinforcing the first line of defense against microbial invasion. The findings, published in Nature Communications with lead authors Amanda Dugan and Deepsing Syangtan from Professor Laura Kiessling's lab, resolve longstanding questions about how the gut maintains its defenses against the hundreds of bacterial species it encounters every day.
Intelectin-2 is a member of a protein family called lectins — molecules that specifically bind to sugar structures. The MIT team discovered that intelectin-2 binds to galactose, a sugar commonly found both in mucin proteins that make up mucus and on the outer membranes of many bacteria. When intelectin-2 encounters bacteria, it latches onto galactose-containing sugars on their outer membranes, crosslinking the bacteria's surfaces and physically restraining them from moving and proliferating. The same binding activity, when it acts on mucins rather than bacteria, crosslinks the protein chains in the mucus layer, making the gel denser and more resistant to bacterial penetration — effectively tightening the gate against bacterial invasion.
The dual mechanism means intelectin-2 operates on two complementary levels simultaneously. It helps maintain the mucus layer as a structural barrier against bacterial intrusion, and if bacteria nonetheless penetrate the mucus, the protein can directly engage and disable the invaders. This redundancy represents a sophisticated antimicrobial strategy that researchers said was unexpected given intelectin-2's relatively simple molecular structure. Both human and mouse versions of the protein showed this broad-spectrum antimicrobial activity, indicating the mechanism is evolutionarily conserved and fundamental to gut health across mammals. The team tested intelectin-2's activity against multiple bacterial species that commonly cause gastrointestinal infections, including strains of E. coli, Salmonella, and Listeria, finding consistent antimicrobial effects against all of them tested.
The discovery is particularly significant for understanding and potentially treating inflammatory bowel disease, which affects approximately 3 million Americans and is believed to involve breakdown of the intestinal barrier, allowing bacteria to penetrate the mucus layer and trigger chronic immune system activation. Patients with Crohn's disease and ulcerative colitis frequently show disrupted mucus layers and altered intelectin expression patterns, though the exact role of intelectin-2 in disease progression had previously been unclear. The new findings suggest that augmenting or restoring intelectin-2 function could be a viable therapeutic strategy for strengthening the intestinal barrier in IBD patients, either through direct administration of the protein, by identifying drugs that stimulate its production, or by developing modified versions with enhanced activity.
Beyond IBD, intelectin-2's broad-spectrum antimicrobial activity could be harnessed in multiple applications. Researchers are exploring whether engineered versions of the protein could be developed as topical antimicrobials for wound care or as additives to prevent bacterial contamination in food processing. The protein's ability to act effectively at physiological temperatures without requiring specialized conditions makes it potentially practical for such applications. The MIT team is now investigating which bacterial pathogens are most susceptible to intelectin-2 and conducting studies to determine whether the protein can effectively combat infections in animal models of intestinal disease, with the goal of establishing a scientific pipeline toward eventual clinical testing in human patients with IBD and other gastrointestinal conditions.
Originally reported by MIT News.